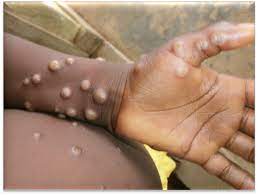
A new study, led by researchers from Liverpool School of Tropical Medicine(U.K.), finds that the monkeypox virus can spread widely within specialist hospital isolation rooms. This presents a new challenge and warning to healthcare settings.
Monkeypox is caused by the monkeypox virus, a zoonotic virus in the genus Orthopoxvirus. Symptoms include fever, swollen lymph nodes, and a rash that forms blisters and then crusts over. As of September 29 (2022), more than 67, 000 infections have been reported globally, with more than 3,400 confirmed cases in the U.K.
This study outcome relates to data that showed in hospital isolation rooms containing patients with monkeypox, viral DNA was found on multiple surfaces, personal protective equipment, and in air samples. For some of the samples, the viral particles were capable of replicating, and therefore could potentially infect other people – both patients, visitors and healthcare professionals.
Viral DNA shed by the patients was found on multiple surfaces throughout the isolation rooms (56 (93 percent) positive by PCR out of 60 samples). In addition, monkeypox virus DNA was also found on personal protective equipment and monkeypox virus DNA was also detected in five out of twenty air samples taken within these isolation rooms.
It was also noted that monkeypox virus capable of replicating in cells under laboratory conditions (an indicator that the virus could infect other people) was identified in two of four PCR-positive samples selected for virus isolation.
This reveals a potential transmission risk and one that is needs to be controlled in hospital settings, although there was no suggestion that transmission of monkeypox virus via aerosols is a common way for the infection to spread from one person to another.


One of the primary transmission risks was attributed to changing bed linen, which appeared to increase the likelihood of monkeypox virus entering the air. The monkeypox virus can be shed into the surrounding environment by shed skin particles and in debris from monkeypox skin lesions and scabs.
It is if additional concern that the virus is relatively hardy and under appropriate conditions can remain infectious on surfaces for weeks, creating a potential infection risk to others.
These results suggest that monkeypox virus shed into a hospitalised patient’s environment poses an infection risk that needs to be managed. The implications include developing protocols so that those who are infected be cared for in isolation rooms, with infection prevention and control precautions that aim to contain potentially infectious virus within the room and protect staff who enter.
The research appears in the journal The Lancet Microbe, titled “Air and surface sampling for monkeypox virus in a UK hospital: an observational study.”
Source: